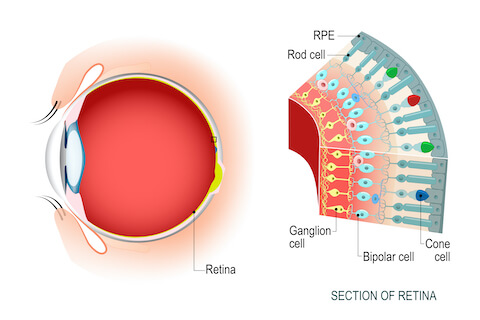
What is a Retinal Detachment or Tear?
Although it may not be obvious when it happens, a retinal detachment occurs when the retina pulls away from its normal position in the eye. This should be in the back of the eye. If the retina does detach, it separates itself from the retinal cells and blood vessels.
These blood vessels are vital to the retina functioning properly since they provide the eye with oxygen and necessary nourishment. If you leave a retinal detachment untreated for too long, it could lead to permanent vision loss in the eye.
A retinal tear is more of a warning sign that a retinal detachment could occur. If a retinal tear is caught early and diagnosed quickly, there is a good chance it will not lead to a retinal detachment. Not all retinal tears need to be treated.
In some cases, they may be low-risk tears, meaning they have no symptoms and do not require treatment. These tears can treat themselves and develop adhesion around the tear.
If you experience a retinal detachment, it is a medical emergency that must be dealt with immediately. Untreated retinal detachments or tears can result in permanent vision loss.
Are There Symptoms of a Retinal Detachment or Tear?
A retinal detachment sounds like it could be painful, but you may not even notice it. Some symptoms or warning signs that a retinal detachment will occur include:
- Seeing more floaters than normal in your field of vision
- Seeing flashes of light, which could occur in one or both of your eyes, known as photopsia
- Experiencing blurred vision
- Experiencing a gradual reduction in your side or peripheral vision
- Seeing a curtain-like shadow that takes up much of your field of vision
With an acute retinal tear, the most common symptom that patients experience are floaters in the affected eye. You may also see flashes of light.
If there is any bleeding in the clear cavity of the eye (known as a vitreous hemorrhage) or any retinal detachment along with the tear, other symptoms may include the same symptoms as above. Often, a retinal tear may not cause any noticeable symptoms.
What Causes a Retinal Detachment or Tear?
There are three different kinds of retinal detachment: rhegmatogenous, tractional, and exudative.
A rhegmatogenous detachment is the most common kind. It is caused by a hole or a tear in the retina that allows fluid to go through and sit under the retina.
This pulls the retina away from its underlying tissues. On the areas where the retina detaches, the blood supply is lost and no longer works, causing the patient to lose their vision.
In most cases, the reason for a rhegmatogenous detachment is because of age. Aging causes the vitreous inside the eye to change. It may lose its consistency, shrink, or become more liquid.
The vitreous is supposed to be able to move and separate from the surface of the retina without complications. If the vitreous separates or starts peeling off the retina, it could tug on the retina with too much force, leading to a retinal tear.
If this is not treated, it could then lead to the vitreous passing through the tear into the space located behind the retina and detaching the retina.
A tractional detachment can occur if scar tissue grows on the retina’s surface. Because of this scar tissue, it causes the retina to pull away from its proper location at the back of the eye.
Tractional detachment is less common and is usually seen in people with diabetes that is not under control or other conditions.
An exudative detachment occurs when fluid accumulates under the retina. Unlike in a tractional or a rhegmatogenous detachment, there are no holes or tears found in the retina.
Instead, an exudative detachment can occur because of injury to the eye, macular degeneration, inflammatory disorders, or tumors.
What Are the Risk Factors for Developing a Retinal Detachment or Tear?
There is no way to say whether someone will or will not develop a retinal detachment or tear, but there are certain factors that increase your risk. They include the following:
- Being over the age of 50 years old
- Already having a previous history of retinal detachment in one eye
- Having a family history of retinal detachment
- Suffering from extreme nearsightedness (myopia)
- Having undergone another eye surgery like cataract surgery
- Having had a severe eye injury previously
- Having an eye disease or disorder like uveitis, retinoschisis, or lattice degeneration (thinning of the peripheral retina)
Concerned about retinal detachment or tears? Shoreline Vision in the Tri-Cities and Muskegon area provides state-of-the-art eye care for patients, including treatment of retinal detachment and tears.






